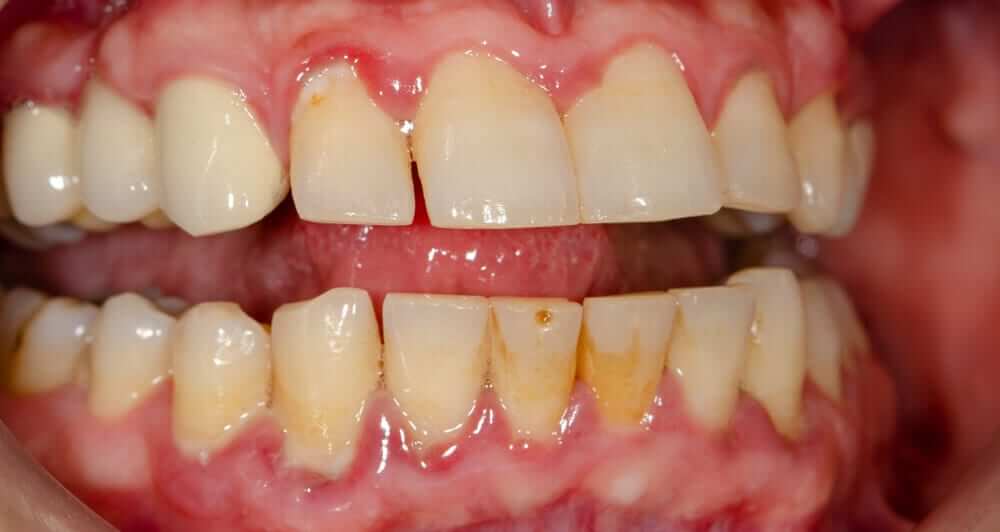
Over one half of all American adults suffer from gingivitis or more advanced periodontal disease conditions affecting the mouth. This number is staggering and considering the close connections between poor oral health and many disease conditions, it should serve as a wake-up call. The long term affects reach much further than just the risk of tooth loss, but can also create an increased risk to cardiovascular disease, liver and kidney problems, and overall digestive disturbances. Current treatment options are limited in regards to the benefits to the patients and lead to months or years of ongoing suffering. Are there better options that might pose a higher level of benefit to the patient, beyond traditionally recommended approaches?
Our teeth are a gift, allowing us to properly chew our food and facilitate the digestion process. Each tooth is surrounded and supported by the gingiva, gum tissue, surrounding ligaments and bone. Gingivitis is a chronic inflammatory condition primarily affecting the gum or gingival tissue. As this condition of gingivitis progresses or worsens over time, it begins to involve deeper structures around the tooth, including ligaments and bone. This is then termed periodontitis or periodontal disease, and the risk of tooth infections and tooth loss dramatically increases.
The clinical signs associated with gingivitis include:
- bleeding gums
- bad breath
- loose teeth
- receding gums
- tooth loss
- toothaches
- mouth ulcers
- mouth pain
These same clinical signs are present in cases of periodontitis or periodontal disease, except that in most the condition is far more progressed or serious.
Causes and Therapy Options for Gingivitis and Periodontal Disease
There is no one cause for gingivitis or periodontal disease in adults or children. These conditions tend to increase in occurrence as we age, for various reasons. The most common cause for gingivitis and periodontal disease is poor oral hygiene. This may be then coupled with various food types that are consumed, which can be irritating to the tissue in the mouth, or foods that lack in proper nutrient provision which support oral health. Other lifestyle factors that come into play include smoking or tobacco usage, along with persistently high stress levels. It is worth mentioning that conditions involving a lowered immune response, may also predispose to developing gingivitis. Those conditions may include ongoing stress, HIV or AIDS, leukemias or cancers, or certain chronic medications. Some women are also predisposed due to hormonal fluctuations associated with menstrual cycles or pregnancy.
Given the number one cause being poor oral hygiene, it then makes sense that the most common therapies implemented include a professional dental cleaning, along with proper daily hygiene which includes teeth brushing, flossing, and certain oral rinses. Other more advanced therapies may include oral medications, prescription rinses, anti-inflammatory medications, and dental restorations.
The good news is that most early stage cases of gingivitis respond very rapidly, often in just a few days with proper care. Other cases, dependent upon the stage of progression, may take much longer or could even persist for months or years, becoming worse over time. This can create months if not years of ongoing oral pain, bleeding, and suffering.
Bacteria and Connections with Gingivitis and Periodontal Disease
Your mouth is home to 200-300 different types of bacterial species. In reality, your mouth contains it’s own specific microbiome, which when in balance promotes proper health. In a state of dysbiosis or imbalance, disease is more common, which includes gingivitis and periodontitis. The most common bacteria associated with tooth decay and periodontal disease is Streptococcus mutans, which is further pushed along in progression by various Lactobacillus, Treponema, Porphyromonas species of bacteria. These two bacterial types are normally present in your mouth, but in certain situations, their levels are increased relative to other groups, which then can create harm.
The pH of your mouth varies dependent upon the food types that you consume or drink. The consumption of highly fermentable foods or food with high sugar contents tends to favor a more acidic oral pH. The more acidic that your mouth becomes, the more likely these ‘bad’ bacterial species can increase in numbers and create harm. It is important to keep in mind that this is not really a true infection, but more so, the oral environment in your mouth has changed, allowing ‘bad’ bacteria to increase in number while lowering the levels of ‘good’ or beneficial bacteria. This is termed a dysbiosis. In some cases, this dysbiosis becomes severe enough, with oral environmental changes, that yeast begin to also increase in number, which is associated with oral Candida infections.
Through modification of your eating and drinking habits, bacterial populations in your mouth can be kept in a more normal balance, especially when coupled with proper oral hygiene habits. Oral rinses or mouthwashes can provide benefits, as many do inhibit Streptococcus mutans, and prevent over growth of this bacteria. However, there are downsides to the mouthwashes or rinses which include killing off other ‘good’ bacteria and also being possibly irritating to the mouth, creating inflammation on some levels.
Triphala and Ayurvedic Medicine to the Rescue for Gingivitis
Triphala is an ancient Ayurvedic herbal blend consisting of three simple ingredients, used for centuries to promote oral and digestive health. This simple blend consists of Terminalia chebula, Terminalia bellerica, and Phyllanthus emblica in specific ratios. The benefits of these herbs, as demonstrated by clinical experience and research include tremendous antioxidant benefit, anti-inflammatory properties, antimicrobial properties, and a mild laxative effect. Triphala has been relied upon traditionally to promote a healthy digestion process, when consumed after meals. This digestive process starts in the mouth, which is just one of many areas that this formula provides clinical benefit.
In many cases of ongoing gingivitis or periodontal disease, it is not uncommon to have prescription anti-bacterial mouthwashes dispensed, which includes a chlorhexidine rinse. Chlorhexidine is a strong anti-microbial solution often used in surgical preparations. In one study, chlorhexidine rinses were compared to triphala rinses in the management of gingivitis. The group of 90 participants demonstrated a marked reduction in bacterial counts and associated oral inflammation equally between the chlorhexidine and triphala groups. This means that the triphala oral rinse group did as well, if not potentially better than the chlorhexidine group, regarding their management of gingivitis.(1)
In another study of undergraduate female students, triphala was also demonstrated to be equally as effective as a chlorhexidine rinse when it came to reduction of dental tartar, gingivitis, and oral inflammation.(2)
In looking at this research data, you may conclude that both are equal in effectiveness, so why would you consider triphala herbal rinse over chlorhexidine mouthwashes? Well, let’s take a look at the side effects listed for the most commonly dispensed oral chlorhexidine mouthwash solution.
- Tooth or tongue staining
- Increased tartar
- Mouth and throat irritation
- Dry mouth
- Unpleasant taste in mouth
- Decreased taste sensation
- Tongue swelling
- Gingivitis
- Mouth sores
Pretty significant right? These side effects may actually contribute to ongoing gingivitis and progression of periodontal disease, rather than resolve it. You have to remember that chlorhexidine is a chemical, which is irritating and damaging, no matter what tissue it is exposed to.
Triphala, on the other hand, demonstrated no side effects in any of the published research trials. Considering the nature of the three herbs in the formula and their noted benefits, side effects would likely not be expected. More so, tissue health would likely be promoted as a result of the anti-microbial properties, antioxidant, and anti-inflammatory potential. These benefits help to protect and promote tissue health, rather than degrade it.
Oral and Digestive Health; Being Proactive and Reactive
Your teeth are a part of your general well being and health. They are essential for chewing of food and the initiation of the digestive process. Bacterial infections that develop in the mouth are closely linked to infections in other areas of the body, including the heart, liver, kidney, and digestive tract. Oral health should never be taken for granted nor should it only be pursued after problems have developed. It is far easier to prevent a health problem, rather than attempting to manage it after the fact.
A proper diet, drink habits, oral hygiene, and utilization of various herbs including triphala help you to reduce the risk of oral health conditions, including tooth decay, gingivitis, and periodontal disease. Triphala has been relied upon for centuries to promote digestive health, and is consumed by many after an evening meal or more often, dependent upon the condition being managed. Triphala demonstrates marked benefit in the potential management of oral health conditions, when used as a mouth rinse, but it could also provide marked benefits from a preventive point of view.
Daily oral health care, including triphala usage, could provide marked benefits when it comes to the health of your mouth. You only get one set of real teeth! Any means of promoting extended health in that area can reap years of benefits.
You can find the triphala herb blend in Cur-OST Tri-GUT Human
Author: Tom Schell, D.V.M., CVCH, CHN
References:
- Pradeep, AR et al. Triphala, a New Herbal Mouthwash for the Treatment of Gingivitis. J Periodontol. 2016, Nov;87(11):1352-1359
- Baratakke, SU et al. Efficacy of Triphala extract and Chlorhexidine Mouth Rinse Against Plaque Accumulation and Gingival Inflammation Among Female Undergraduates. Indian J Dent Res. 2017, Jan-Feb;28(1):49-54